Rapid Fire Session
Prognostic Value of CMR-Derived Indices in Heart Transplant Recipients for Multi-Year Outcomes

Courtney J. Pfister, BSc
Student
Northwestern University
Chicago, Illinois, United States
Courtney J. Pfister, BSc
Student
Northwestern University
Chicago, Illinois, United States- KL
Kai Lin, MD
Research Associate Professor
Northwestern University Feinberg School of Medicine, United States - RS
Roberto Sarnari, MD
Clinical Research Associate
Northwestern University Feinberg School of Medicine
Chicago, Illinois, United States 
Daniel C. Lee, MD
Professor of Medicine and Radiology
Northwestern University Feinberg School of Medicine
Chicago, Illinois, United States
James Carr, MD
Chair
Northwestern University Feinberg School of Medicine
chicago, Illinois, United States
Presenting Author(s)
Primary Author(s)
Co-Author(s)
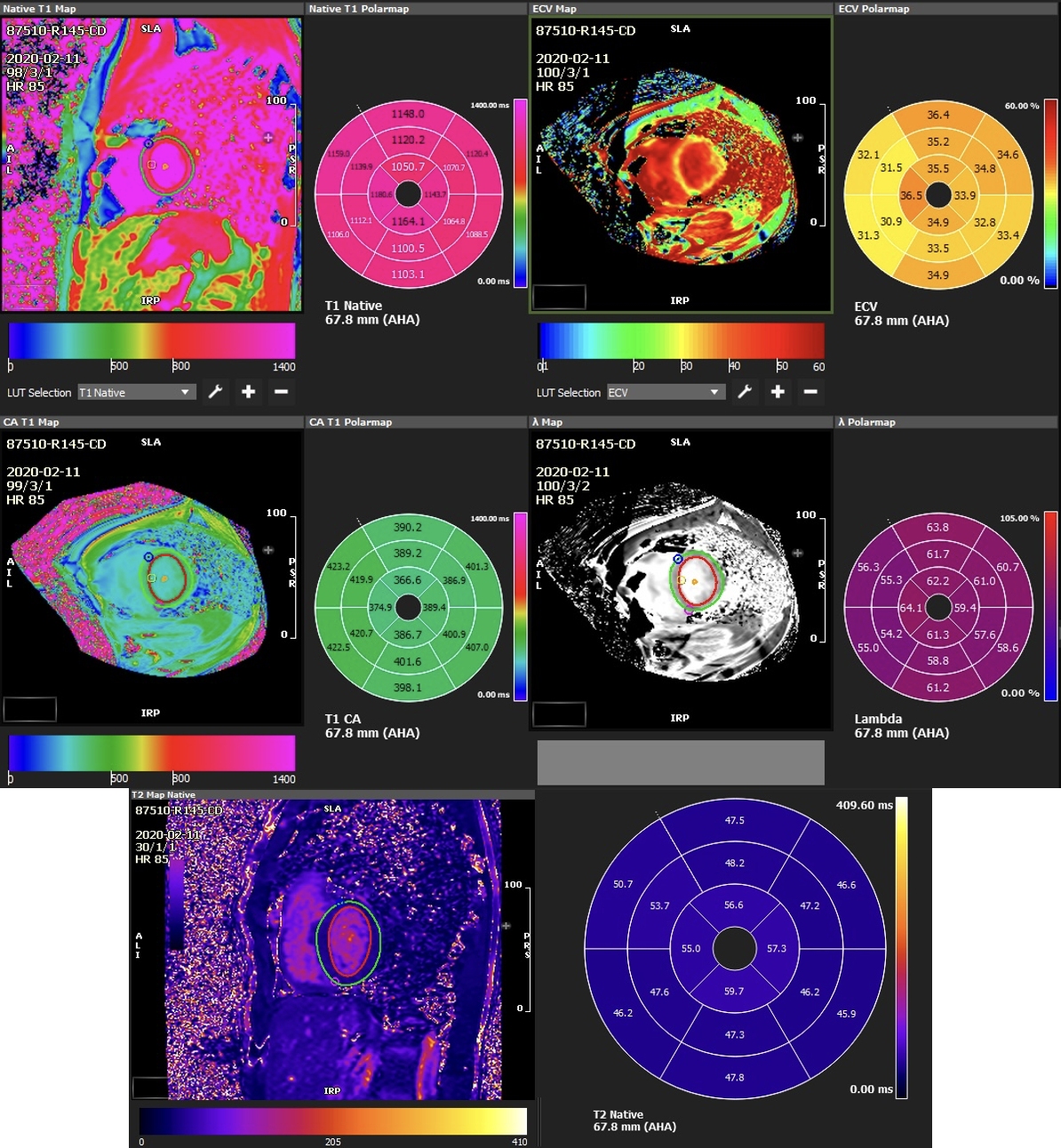
Methods: 171 heart transplant (HTx) recipients underwent comprehensive multi-parametric cardiac magnetic resonance imaging (CMR). Left and right ventricular (LV, RV) and atrial (LA, RA) volumes were obtained at each cardiac time frame by summing the areas of all slices from the base to the apex of the heart. From these data, end-diastolic volume (LVEDV, RVEDV), end-systolic volume (LVESV, RVESV), stroke volume (LVSV, RVSV), cardiac output (LVCO, RVCO), cardiac index (LVCI, RVCI), ejection fraction (LVEF, RVEF), and LV mass (LVM) were calculated. Myocardial density was assumed to be 1.05 g/mL. Myocardial tissue characteristics, including T1 and T2 relaxation times, were measured, and extracellular volume (ECV) was derived from pre- and post-contrast T1 values. Representative CMR mapping is seen in Figure 1. Logistic regression and cox proportional hazards (CPH) models were used to determine whether MRI-derived cardiac indices can be used to predict clinical events. The clinical outcomes utilized are seen in Table 1. Statistical analyses were conducted using SPSS (version 22.0; IBM Corp., Armonk, NY).
Results: Our cohort contained 171 heart transplant (HTx) recipients (105 males, mean age: 48 years, range 18–80 years). Different MRI-derived indices demonstrated variable prognostic performance across logistic and CPH models, as summarized in Table 2. All-cause mortality was 3.5% (n=6), 5.3% (n=9), and 10.5% (n=18) at 1, 3, and 5 years after MRI, respectively, with a mean f.u. time of 100±103 mo. MACE occurred in 14.6% (n=25), 23.4% (n=40), and 25.1% (n=43) and at 1, 3, and 5 years (mean f.u. 81 ± 81 mo.), while CVEs occurred in 29.2% (n=50), 59.1% (n=101) and 70.8% (n=121), respectively (mean f.u. 39±39 mo.). Pre- and post- contrast T1 and T2 were significant predictors of reduced survival (p < .05). Elevated myocardial T2 was a significant predictor of all-cause mortality at 1-year post-MRI, while elevated LVM (left ventricular mass) was a significant predictor of mortality at 3 years (p < .05).
Conclusion: The prognostic performance of CMR-derived indices in heart transplant recipients varies depending on clinical outcomes and include both global LV function as well as tissue parameters (T1, T2). The findings underscore the importance of a multiparametric imaging approach in passing structural and functional abnormalities of the HTx allograft.
Table 1. Clinical outcomes and definitions assessed by logistic regression and Cox proportional hazards (CPH) models.
Model | Outcome Type | Specific Outcomes Evaluated |
Logistic Regression | All-cause mortality | Alive status at 1-, 3-, and 5-years post-MRI |
Major Adverse Cardiac Events (MACE) | Occurrence at 1-, 3-, and 5- years post-MRI | |
Cardiovascular Events (CVEs) | Occurrence at 1-, 3-, and 5- years post-MRI | |
Cox Proportional Hazards (CPH) | Survival | For patients alive at follow-up, time from index MRI to chart review in the electronic medical record (Epic) |
Survival free of MACE | Binary: event vs. no event during follow-up | |
Survival free of CVEs | Binary: event vs. no event during follow-up |
Clinical outcomes assessed by logistic regression (events at 1, 3, and 5 years) and CPH models (time-to-event survival, MACE, and CVEs). MACE is a composite of cardiovascular death, myocardial infarction, hospitalization for heart failure, or revascularization. CVEs include any emergency department visit, hospitalization, or death that cannot clearly be attributed to non-cardiovascular causes (e.g. trauma, accidents). Table 2. Post-HTx clinical outcomes with follow-up, event rates, and significant CMR predictors.
HTx Outcome | Mean follow-up (months) | Logistic Regression Timepoint (n, %) | Significant CMR Predictors | ||
1-year | 3-year | 5-year | |||
All-cause mortality | 100 ± 103 | 6 (3.5%) | 9 (5.3%) | 18 (10.5%) | Logistic: T2 (1-year), LVM (3-year) CPH: Pre- and post-T1, T2 |
MACE | 81 ± 81 | 25 (14.6%) | 40 (23.4%) | 43 (25.1%) | NA |
CVE | 39 ± 39 | 50 (29.2%) | 101 (59.1%) | 121 (70.8%) | NA |
Mean follow-up time (± SD) is reported in months from index MRI to the outcome of interest (e.g., death) or, if no event occurred, to the time of chart review. Event counts (n) and percentages are shown for all-cause mortality, MACE, and CVEs at 1, 3, and 5 years. NA = no significant CMR-derived predictors. Significant CMR predictors included T2 for 1-year all-cause mortality, LVM for 3-year all-cause mortality, and pre-/post-contrast T1 and T2 on CPH analysis. Limited by the space and topic of this study, we are not listing non-MRI-derived cardiovascular indices that can be used to predict the outcomes.Figure 1. Multiparametric CMR maps at index scan. Example native and post-contrast T1, extracellular volume (ECV), and T2 maps from a representative subject at index CMR scan. Top Row: native T1 and ECV maps with corresponding polar plots. Middle Row: Post-contrast T1 map with polar plots. Bottom row: T2 map and polar plot.