Rapid Fire Session
Cardiac MRI-Guided Assessment of Defibrillator Benefit in Cardiac Resynchronization Therapy for Non-Ischemic Cardiomyopathy

Anna Charlotte Tuinman, MD
PhD candidate, MD
Amsterdam Medical Center
Amsterdam, Noord-Holland, Netherlands
Anna Charlotte Tuinman, MD
PhD candidate, MD
Amsterdam Medical Center
Amsterdam, Noord-Holland, Netherlands
Luuk H.G.A Hopman, PhD
Postdoctoral Researcher Cardiology
Amsterdam UMC
Amsterdam, Noord-Holland, Netherlands- Sv
Sophie van der Geest
Graduate student
Amsterdam UMC, Zuid-Holland, Netherlands - Pv
Philippe van Rosendael, MD, PhD
MD, PhD
Leiden University Medical Center, Netherlands - MG
Marco J.W Götte, MD, PhD
MD, PhD
Stephenson Cardiac Imaging Centre
Calgary, Alberta, Canada - Vv
Vokko van Halm, MD, PhD
dr.
Amsterdam Medical Center, Netherlands - CA
Cornelis Allaart, MD, PhD
VU university medical center, Amsterdam, Netherlands
Presenting Author(s)
Primary Author(s)
Co-Author(s)
Methods: In this retrospective cohort, NICM patients with ejection fraction < 35% receiving de novo CRT-D between January 2009 - April 2022 and had a pre-implantation CMR scan were included. CMR was used to assess LGE presence, distribution and burden, and dyssynchrony was quantified on a mid-ventricular cine slice using the systolic stretch index (SSI) [2]. The primary outcome was time to first appropriate device therapy (ADT) and secondary outcome was all-cause mortality. Follow-up continued until March 2025.
Results: Of the 115 CRT-D patients, 101 had images available for LGE analysis, of whom 45 (44.6%) were LGE-positive. In LGE-positive patients, LGE was present in median 2 segments (IQR 2–3); 35.6% had an isolated midwall septal stripe, 8.9% only had inferior hinge-point LGE. In 86 patients, scans were available for SSI analysis, median SSI was 8.96 (IQR 5.2).
Over a median follow-up of 5.0 years (IQR 6.0), 9.7% experienced ADT, with no difference between LGE-positive (6.7%) and LGE-negative (11.7%, P=0.91), or between high (11.6%) and low SSI (9.3%, P=0.73). Among LGE-positive patients, those with ADT demonstrated a significantly greater LGE burden, reflected by the number of involved segments, than those without ADT (median 6 vs. 2; P=0.02).
During follow-up, 29.2% died; mortality did not differ by LGE presence (24.4% vs 32.1%, P=0.40) or SSI (37.2% vs 30.2%, P=0.49). Neither LGE (HR 0.753; P=0.48) nor SSI (HR 0.991; P=0.88) was associated with mortality. In multivariable analysis, age (HR 1.082; P=0.002) and creatinine (HR 1.010; P=0.01) were independently associated with mortality.
Conclusion: In NICM patients undergoing CRT-D implantation for primary prevention, neither pre-implantation LGE presence nor mechanical dyssynchrony was associated with ADT or all-cause mortality. However, among LGE-positive patients, those who experienced ADT had a significantly higher LGE burden. These findings suggest that the extent of LGE may be relevant for risk stratification between CRT-D and CRT-P in selected patients, but larger studies are needed to confirm this observation.
Univariable and Multivariable analysis Appropriate Device Therapy and mortality
| Univariable | Multivariable |
| Univariable | Multivariable | ||||||
HR (95% CI) | p-value | HR (95% CI) | p-value |
| HR (95% CI) | p-value | HR (95% CI) | p-value | |||
Age (years) | 0.993 (0.936 – 1.055) | 0.83 |
|
| Age (years) | 1.098 (1.047 – 1.152) | < .001 | 1.082 (1.029 – 1.136) | 0.002 | ||
Sex (male) | 0.338 (0.091 – 1.253) | 0.11 |
|
| Sex (male) | 0.663 (0.336 – 1.307) | 0.24 |
|
| ||
BMI (kg/m2) | 1.110 (0.981 – 1.255) | 0.10 |
|
| BMI (kg/m2) | 1.022 (0.945 – 1.105) | 0.59 |
|
| ||
Hypertension | 1.331 (0.621– 2.852) | 0.46 |
|
| Hypertension | 1.017 (0.646 – 1.601) | 0.94 |
|
| ||
Diabetes | 1.038 (0.281 – 3.837) | 0.96 |
|
| Diabetes | 1.093 (0.491 – 2.435) | 0.83 |
|
| ||
Hypercholesteremia | 1.411 (0.723 – 2.755) | 0.31 |
|
| Hypercholesteremia | 1.144 (0.770 – 1.700) | 0.51 |
|
| ||
History to AF | 1.598 (0.988 – 2.582) | 0.06 | 3.044 (0.838 – 11.053) | 0.09 | History to AF | 1.318 (0.934 – 1.861) | 0.12 |
|
| ||
Creatinine (µmol/L) | 1.008 (0.996 – 1.020) | 0.21 |
|
| Creatinine (µmol/L) | 1.012 (1.005 – 1.019) | < .001 | 1.010 (1.002 – 1.018) | 0.01 | ||
NYHA class | 0.372 (0.151 – 0.917) | 0.03 | 0.095 (0.007 – 1.396) | 0.09 | NYHA class | 0.846 (0.525 – 1.365) | 0.49 |
|
| ||
LVEF (%) | 1.005 (0.934 – 1.081) | 0.90 |
|
| LVEF (%) | 0.979 (0.938 – 1.021) | 0.32 |
|
| ||
QRS duration (msec) | 1.001 (0.970 – 1.032) | 0.96 |
|
| QRS duration (msec) | 1.004 (0.986 – 1.023) | 0.64 |
|
| ||
Non-LBBB | 0.536 (0.161 – 1.789) | 0.31 |
|
| Non-LBBB | 0.471 (0.233 – 0.954) | 0.04 | 0.488 (0.221 – 1.075) | 0.08 | ||
Amiodarone | 1.263 (0.163 – 9.794) | 0.82 |
|
| Amiodarone | 1.295 (0.395 – 4.249) | 0.67 |
|
| ||
Beta blocker | 0.660 (0.178 – 2.441) | 0.53 |
|
| Beta blocker | 1.171 (0.484 – 2.834) | 0.73 |
|
| ||
ACE or ATII antagonist | 0.666 (0.143 – 3.043) | 0.60 |
|
| ACE or ATII antagonist | 0.573 (0.250 – 1.316) | 0.19 |
|
| ||
MRA | 2.169 (0.651 – 7.222) | 0.21 |
|
| MRA | 0.962 (0.488 – 1.894) | 0.91 |
|
| ||
LGE on CMR | 0.602 (0.150 – 2.410) | 0.47 |
|
| LGE on CMR | 0.702 (0.331 – 1.492) | 0.36 |
|
| ||
LGE pattern | 2.458 (0.265 – 22.794) | 0.43 |
|
| LGE pattern | 0.889 (0.327 – 2.419) | 0.82 |
|
| ||
LGE burden | 1.085 (0.898 – 1.310) | 0.40 |
|
| LGE burden | 0.943 (0.781 – 1.138) | 0.54 |
|
| ||
SSI on CMR | 1.050 (0.870 – 1.266) | 0.61 |
|
| SSI on CMR | 0.998 (0.895 – 1.113) | 0.97 |
|
| ||
* Univariable and multivariable analyses of ADT and mortality during follow-up. Hazard ratios (HR) with 95% confidence intervals (CI) and p-values are presented for each variable.
Abbreviations: ADT = appropriate device therapy; BMI = body mass index; AF = atrial fibrillation; NYHA = New York Heart Association; LVEF = left ventricular ejection fraction; LBBB = left bundle branch block; ACE = angiotensin converting enzyme; ATII = angiotensin II; MRA = mineralocorticoid receptor antagonist; LGE = late gadolinium enhancement; CMR = cardiac magnetic resonance; SSI = systolic stretch index. Figure 1. LGE Patterns and Mechanical Dyssynchrony in NICM Patients Undergoing CRT-D Implantation. Distribution of late gadolinium enhancement (LGE) patterns and systolic stretch index (SSI) in non-ischemic cardiomyopathy patients undergoing CRT-D implantation. Pie chart shows the proportion of LGE patterns; scatter plot displays SSI distribution above and below the median of 8.96. Median follow-up was 5 years.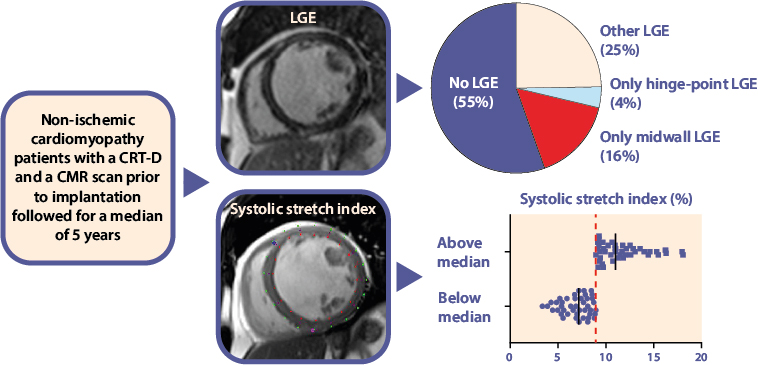 Figure 2. Kaplan Meier curves for ADT and mortality in NICM CRT-D patients. Panel A: Kaplan-Meier analysis stratified by LGE-positive and LGE-negative CRT-D patients, showing the occurrence of appropriate device therapy (ADT), p = 0.63. Panel B: Kaplan-Meier analysis stratified by LGE-positive and LGE-negative CRT-D patients, showing mortality, p = 0.35. Panel C: Kaplan-Meier analysis stratified by SSI high and SSI low CRT-D patients, showing the occurrence of ADT, p = 0.78. Panel D: Kaplan-Meier analysis stratified by SSI high and SSI low CRT-D patients, showing the occurrence of mortality, p = 0.69.
Figure 2. Kaplan Meier curves for ADT and mortality in NICM CRT-D patients. Panel A: Kaplan-Meier analysis stratified by LGE-positive and LGE-negative CRT-D patients, showing the occurrence of appropriate device therapy (ADT), p = 0.63. Panel B: Kaplan-Meier analysis stratified by LGE-positive and LGE-negative CRT-D patients, showing mortality, p = 0.35. Panel C: Kaplan-Meier analysis stratified by SSI high and SSI low CRT-D patients, showing the occurrence of ADT, p = 0.78. Panel D: Kaplan-Meier analysis stratified by SSI high and SSI low CRT-D patients, showing the occurrence of mortality, p = 0.69..jpg)

