Early Career Award Session
Virtual Recording
One-click AI-assisted analysis of bright- and black-blood LGE and T2 mapping in acute STEMI patients

Victor de Villedon de Naide, MSc
PhD student
Bordeaux University - INSERM U1045
Bordeaux, Aquitaine, France
Victor de Villedon de Naide, MSc
PhD student
Bordeaux University - INSERM U1045
Bordeaux, Aquitaine, France- EG
Edouard Gerbaud, MD, PhD
Cardiac Intensive Care Unit, Groupe Hospitalier Sud, CHU de Bordeaux, Pessac, France, France
- SV
Sane Viola
Engineer
IHU Liryc, Université de Bordeaux, France 
Thaïs Genisson, MSc
PhD student
IHU Liryc, Université de Bordeaux
Bordeaux, Aquitaine, France
Kalvin Narceau, MSc
Phd student
Bordeaux University - INSERM U1045
Pessac, Aquitaine, France- EB
Ewan Barel
Engineer
IHU Liryc, Université de Bordeaux, France - TR
Théo Richard, MSc
Engineer
IHU LIRYC, Heart rhythm disease institute, Université de Bordeaux – INSERM U1045, Avenue du Haut Lévêque, 33604, Pessac, France
Bordeaux, Aquitaine, France - PJ
Pierre Jaïs, MD, PhD
PROF/PhD
Hôpital Cardiologique du Haut-Lévêque, CHU de Bordeaux
Bordeaux, Aquitaine, France - MS
Matthias Stuber, PhD
Professor/Director
CIBM/CHUV/UNIL
Lausanne, Switzerland - HC
Hubert Cochet, MD, PhD
Professor
Bordeaux University - INSERM U1045
Bordeaux, Aquitaine, France .jpg)
Aurelien Bustin, FSCMR
Research Associate
Department of Cardiovascular Imaging, Hôpital Cardiologique du Haut-Lévêque, CHU de Bordeaux, Avenue de Magellan, Pessac, France; IHU LIRYC, Electrophysiology and Heart Modeling Institute, Université de Bordeaux – INSERM U1045, Avenue du Haut Lévêque, Pessac, France; Department of Diagnostic and Interventional Radiology, Lausanne University Hospital and University of Lausanne, Lausanne, Switzerland
Bordeaux, Aquitaine, France
Presenting Author(s)
Primary Author(s)
Co-Author(s)
Methods: Sequence: SPOT-MAPPING employs an ECG-triggered 2D single-shot sequence alternating between bright- and black-blood LGE images2. Incremental T2-preparation durations in the bright-blood beats (0, 27, 35, 40, 55ms) enable generation of T2 maps, yielding co-registered datasets for anatomy, scar, and oedema assessment within a single acquisition (Fig.1).
Processing: Automated left ventricular (LV) segmentation and right ventricular insertion points detection were performed on bright-blood images, using combined Transformer3 and U-Net4 models trained on 400 independent patients5. LV contours were then propagated to black-blood images for automated scar segmentation (histogram-based thresholding), and to T2 maps for T2 quantification according to the AHA 16-segment model (Fig.1).
Experiments: Ten acute STEMI patients (9 male, age 58±14yo) underwent CMR at 1.5T (Siemens Magnetom Aera) 4-7 days after primary PCI. Protocol included reference T2 mapping, PSIR, and SPOT-MAPPING sequences. Agreement between automated and manual analysis was assessed using Dice coefficients, paired t-tests, Bland-Altman analysis, and bias (95% CI). Parameters including scar volume (g), burden (%LV mass) and transmurality (%), T2 values at the segmental, slice, and patient levels, processing time and segmentation failure rates were measured.
Results: High agreement with manual reference was achieved for automated LV wall segmentation (Dice 87.2±1.3%, slice failure rate 5.9%) (Table 1). Scar segmentation accuracy was moderate-to-high (Dice 68.3±8.2%, slice failure rate 30%). T2 quantification demonstrated excellent agreement at segment, slice and patient levels (mean bias: -2.5ms to -2.9ms). Automated analysis reduced processing time from >20min (manual) to < 0.1min. Representative segmentations and T2-map Bullseyes (Fig. 2) confirmed precise localisation of scar and oedema.
Conclusion: AI-assisted SPOT-MAPPING enables fast and automated quantification of myocardial scar and oedema in a single CMR acquisition in acute STEMI patients. Although scar segmentation failures remain a limitation, these findings support further refinement and large-scale validation in clinical and research applications.
Quantitative comparison of manual and automated SPOT-MAPPING for myocardial scar and oedema assessment. Comparison of LV wall volume, Dice scores, scar volume, scar burden, scar transmurality, T2 values at segment/slice/patient levels, segmentation failure rates, and processing times, with bias and 95% confidence intervals. Abbreviations: LV, left ventricle; STEMI, ST-elevation myocardial infarction; N/A, not applicable.
| Manual Segmentation | Automated Segmentation | P-value | Bias (95% CI) | Notes |
LV wall volume (mL) | 95.9 ± 29.3 | 92.1 ± 28.1 | 0.737 | -3.8 (-5.8 to -1.8) | - |
LV wall Dice score (%) | N/A | 87.2 ± 1.3 | N/A | N/A | vs. manual ground truth |
Scar volume (mL) | 17.6 ± 20.1 | 10.9 ± 8.5 | 0.285 | -6.7 (-9.6 to -3.7) | - |
Scar burden (% of LV mass) | 31.8 ± 13.1 | 28.7 ± 6.6 | 0.510 | -3.1 (-5.7 to -0.6) | - |
Scar transmurality (%) | 68.0 ± 8.0 | 63.0 ± 7.5 | 0.172 | -5.0 (-7.7 to -2.2) | - |
Scar Dice score (%) | N/A | 68.3 ± 8.2 | N/A | N/A | vs. manual ground truth |
T2 values – segment basis (msec) | 61.9 ± 12.5 | 59.3 ± 12.3 | 0.037 | -2.5 (-2.8 to -2.3) | - |
T2 values – slice basis (msec) | 63.0 ± 11.2 | 60.3 ± 10.5 | 0.076 | -2.7 (-3.1 to -2.4) | - |
T2 values – patient basis (msec) | 63.6 ± 6.4 | 60.8 ± 6.8 | 0.277 | -2.9 (-3.5 to -2.3) | - |
Failure rate scar segmentation (% affected slices) | 0.0% | 30.0% | N/A | N/A | defined as unusable segmentation |
Failure rate LV segmentation (% affected slices) | 0.0% | 5.9% | N/A | N/A | defined as unusable segmentation |
Processing time (min) | >20.0 | < 0.1 | < 0.001 | N/A | - |
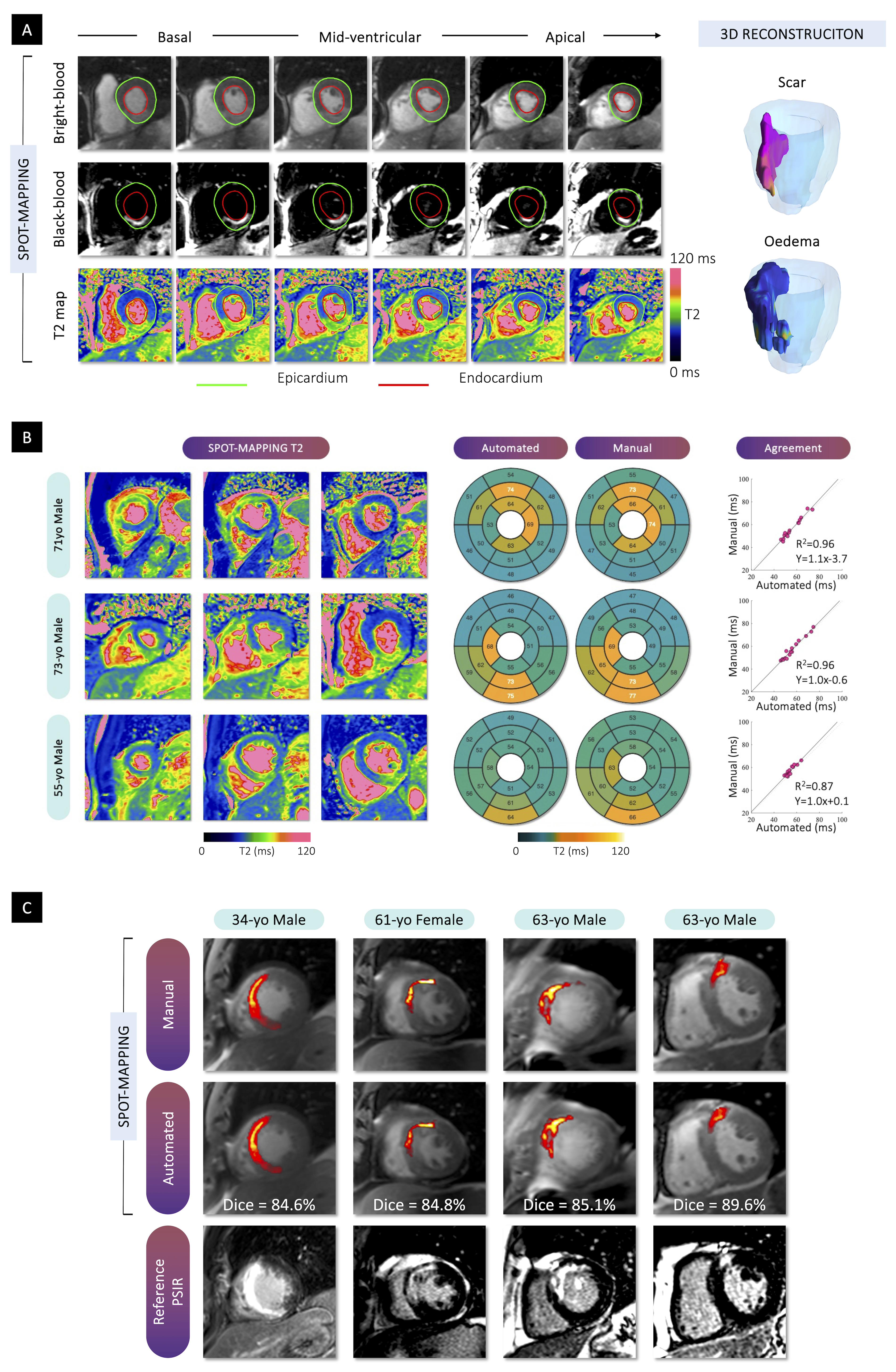
.png) Representative examples of automated versus manual quantification of myocardial scar and oedema using SPOT-MAPPING. A) Representative basal, mid-ventricular, and apical slices from SPOT-MAPPING, including bright-blood, black-blood, and T2 maps, demonstrate regional detection of myocardial oedema and scar, with 3D reconstructions showing spatial distribution. B) Comparison of automated vs. manual segmental T2 quantification in multiple patients, with bullseye plots and scatter plots showing high correlation and agreement across T2 values. C) Scar segmentation overlays from SPOT-MAPPING (manual and automated) compared to PSIR reference images in multiple patients, with Dice coefficients demonstrating strong concordance between automated and manual methods.
Representative examples of automated versus manual quantification of myocardial scar and oedema using SPOT-MAPPING. A) Representative basal, mid-ventricular, and apical slices from SPOT-MAPPING, including bright-blood, black-blood, and T2 maps, demonstrate regional detection of myocardial oedema and scar, with 3D reconstructions showing spatial distribution. B) Comparison of automated vs. manual segmental T2 quantification in multiple patients, with bullseye plots and scatter plots showing high correlation and agreement across T2 values. C) Scar segmentation overlays from SPOT-MAPPING (manual and automated) compared to PSIR reference images in multiple patients, with Dice coefficients demonstrating strong concordance between automated and manual methods.