Rapid Fire Session
Prognostic Value of Right Ventricular Function for Heart Failure in Hypertrophic Cardiomyopathy with Latent Obstruction

Alexander Schulz, MD
Dr.
Harvard Medical School / BIDMC
Berlin, Berlin, Germany- WL
Willemijn Leiner
Research Intern
Harvard Medical School, United States - LP
Lily Peng
Research Assistant
Harvard Medical School, Massachusetts, United States - ER
Ethan Rowin
Doctor
Lahey Hospital, United States 
Amine Amyar, PhD
Instructor in medicine
Harvard Medical School - Beth Israel Deaconess Medical Center
Boston, Massachusetts, United States
Warren J. Manning, MD
Professor
Harvard Medical School
Boston, Massachusetts, United States- MM
Martin S Maron, MD
Cardiologist
beth israel lahey health, Massachusetts, United States - RN
Reza Nezafat, PhD
Professor
Harvard Medical School
Boston, Massachusetts, United States
Presenting Author(s)
Primary Author(s)
Co-Author(s)
Methods: In a large multicenter cohort of 1,333 patients with obstructive HCM who underwent CMR between 2003 and 2023, we identified 284 patients with NYHA class I/II symptoms, preserved LVEF (≥50%), and no prior septal reduction therapy (SRT), who had an LVOT gradient < 30 mmHg at rest but ≥30 mmHg during provocation. Biventricular volumes and function were quantified, and LGE was manually assessed. Feature tracking analysis was performed on four-chamber cine images using QStrain (Medis 4.0.70.4, Leiden, The Netherlands) to derive RV global longitudinal strain (GLS) and free wall strain (Figure 1).The primary endpoint was a composite of HF progression (NYHA class III/IV), new LVEF < 50%, or SRT. Univariable Cox regression analyses were performed including demographical, echocardiographic and CMR variables. Variables with p< 0.05 were entered into multivariable Cox regression models. Kaplan–Meier analysis was used to visualize the prognostic relevance of RV strain, with the optimal cutoff determined by Youden’s index.
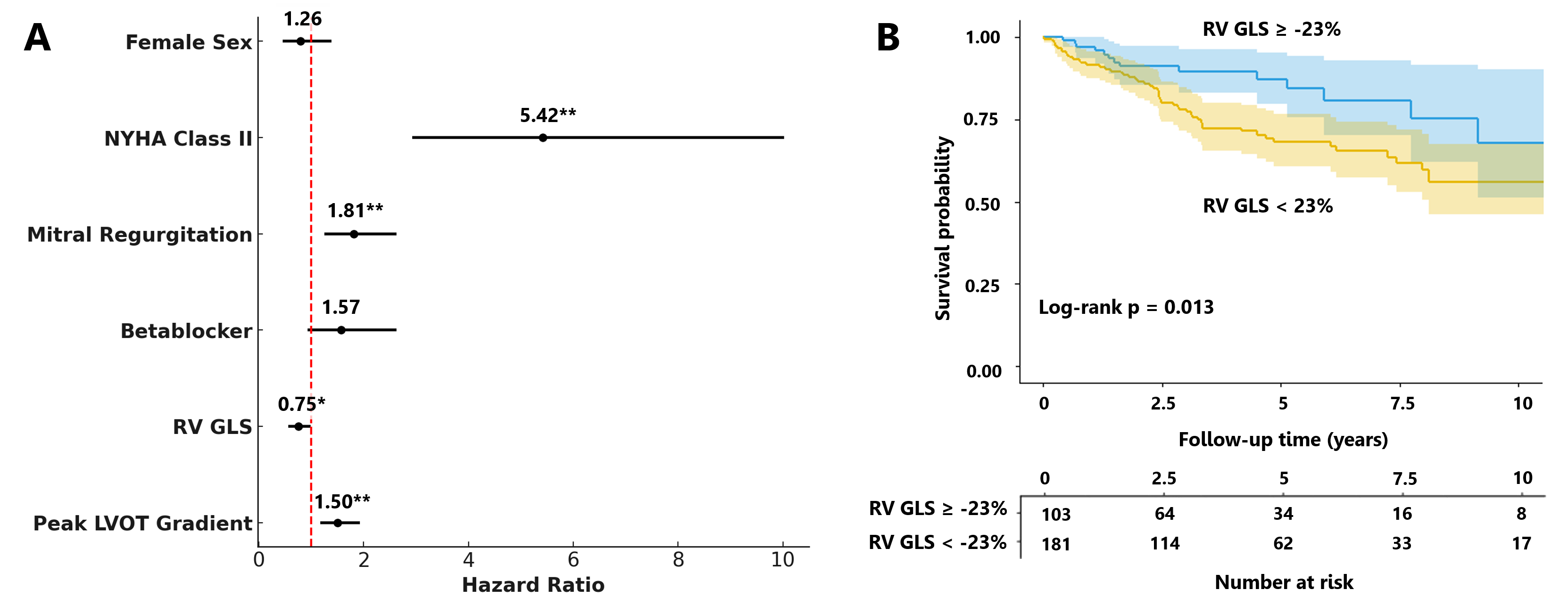
Results: Over a mean follow-up of 5.0 ± 3.3 years, 69 patients (24%) experienced HF events. Compared with event-free patients, those with HF events were more often female, more frequently in NYHA class II at baseline, had higher peak LVOT gradients, and more often presented with mitral regurgitation. They were also more frequently treated with beta-blockers and demonstrated lower RV GLS and RV free wall strain, whereas no other differences in biventricular volumes or function were observed (Table 1). In regression analyses, RV GLS emerged as an independent predictor of HF events, alongside NYHA class II, greater severity of mitral regurgitation, and higher peak LVOT gradient (Figure 2A). At an optimal cutoff of –23%, patients with lower RV GLS had significantly higher probability of HF Events (Figure 2B).
Conclusion: In HCM patients with provocable LVOT obstruction, RV GLS as assessed by CMR feature tracking emerged as an independent predictor of adverse HF events, highlighting the importance of comprehensive evaluation of biventricular coupling in this population.
Table 1: Patient Characteristics and CMR Parameters
Patient characteristics and medical history | No HF Event (n=215) | HF Event (n=69) | p-value |
Sex (male) | 78.1% (168) | 60.9% (42) | 0.004 |
Age at initial visit (years) | 48.57 ± 16.62 | 49.91 ± 14.40 | 0.519 |
Body mass index (kg/m2) | 29.29 ± 5.54 | 30.33 ± 5.41 | 0.183 |
NYHA Class II | 39.5% (85) | 79.7% (55) | < 0.001 |
Atrial fibrillation | 13.0% (28) | 13.0% (9) | 0.997 |
Arterial hypertension | 38.6% (83) | 33.3% (23) | 0.431 |
Coronary artery disease | 6.0% (13) | 4.3% (3) | 0.594 |
Family history of HCM | 20.9% (45) | 17.4% (12) | 0.523 |
Positive record of genetic mutation | 5.6% (12) | 4.3% (3) | 0.69 |
Apical aneurysm | 1.4% (3) | 0.0% (0) | 0.324 |
Mitral regurgitation |
|
|
|
Grade 1 | 29.8% (64) | 31.9% (22) | 0.739 |
Grade 2 | 1.9% (4) | 11.6% (8) | 0.001 |
Grade 3 | 0 (0.0%) | 0 (0.0%) | n/a |
Grade 4 | 0 (0.0%) | 0 (0.0%) | n/a |
Peak LVOT Gradient |
|
|
|
30-49 mmHg | 30.7% (66) | 15.9% (11) | 0.016 |
50-85 mmHg | 43.3% (93) | 40.6% (28) | 0.696 |
>85 mmHg | 26.0% (56) | 43.5% (30) | 0.006 |
Betablocker | 43.3% (93) | 63.8% (44) | 0.003 |
Calcium Channel Blockers | 19.5% (42) | 18.8% (13) | 0.899 |
ACE-Inhibitor/ ARB | 22.3% (48) | 18.8% (13) | 0.54 |
Disopyramide | 0.9% (2) | 1.4% (1) | 0.714 |
CMR | |||
Maximum WT (mm) | 17.70 ± 4.15 | 17.83 ± 3.92 | 0.815 |
LV mass index (g/m2) | 73.69 ± 23.59 | 73.83 ± 25.42 | 0.968 |
LA diameter (mm) | 38.67 ± 8.52 | 39.61 ± 8.33 | 0.417 |
LV end diastolic volume index (ml/m2) | 76.75 ± 16.41 | 75.36 ± 18.10 | 0.573 |
LV stroke volume index (ml/m2) | 51.15 ± 11.04 | 51.29 ± 12.03 | 0.933 |
LV ejection fraction (%) | 66.84 ± 6.67 | 68.12 ± 7.62 | 0.212 |
RV end diastolic volume index (ml/m2) | 69.50 ± 17.52 | 66.60 ± 17.90 | 0.244 |
RV stroke volume index (ml/m2) | 40.40 ± 10.85 | 39.08 ± 11.39 | 0.407 |
RV ejection fraction (%) | 58.57 ± 8.38 | 58.72 ± 7.59 | 0.897 |
RV GLS (%) | -24.57 ± 5.56 | -26.79 ± 4.70 | 0.001 |
RV Free Wall Strain (%) | -31.82 ± 7.22 | -34.34 ± 6.48 | 0.007 |
LGE presence | 46.0% (99) | 43.5% (30) | 0.709 |
Relative LGE mass (%) | 2.19 ± 4.04 | 1.28 ± 2.26 | 0.022 |
WT – Wall thickness, LVOT – Left ventricular outflow tract, ARB – Angiotensin II receptor blocker, LV/RV – Left/Right ventricle, LA – Left atrium, GLS – Global longitudinal strain, LGE – Late gadolinium enhancementFigure 1. Example of right ventricular feature tracking analysis in a patient with hypertrophic cardiomyopathy. Left: RV contouring for feature tracking analysis. Right: Corresponding RV strain curve. RA/LA = right/left atrium; LV/RV = left/right ventricle..png) Figure 2. Predictors of heart failure events (A) and Survival plot stratified by right ventricular global longitudinal strain. Forrest plots of multivariable Cox regression analysis and Kaplan–Meier curves for HF event–free survival, stratified by RV GLS (cut-off of -23%) * p<0.05, ** p<0.01
Figure 2. Predictors of heart failure events (A) and Survival plot stratified by right ventricular global longitudinal strain. Forrest plots of multivariable Cox regression analysis and Kaplan–Meier curves for HF event–free survival, stratified by RV GLS (cut-off of -23%) * p<0.05, ** p<0.01