Early Career Award Session
Virtual Recording
Rapid quantification of stress/rest myocardial blood volume reserve using ferumoxytol-enhanced CMR: New technique and preclinical results at 0.55T

Hazar Benan Unal, PhD
Postdoctoral Research Associate
Laboratory for Translational Imaging of Microcirculation, Purdue University
Indianapolis, Indiana, United States
Hazar Benan Unal, PhD
Postdoctoral Research Associate
Laboratory for Translational Imaging of Microcirculation, Purdue University
Indianapolis, Indiana, United States- SZ
Shahriar Zeynali, MSc
PhD Candidate
Indiana University School of Medicine
Indianapolis, Indiana, United States - AM
Arian M. Sohi, BSc
PhD Student
Laboratory for Translational Imaging for Microcirculation, Weldon School of Biomedical Engineering, Purdue University
Indianapolis, Indiana, United States - EA
Eric Anttila, PhD
Research Engineer
MED Institute, United States 
Rohan Dharmakumar, PhD
Executive Director
Indiana University School of Medicine
Indianapolis, Indiana, United States
David Gross, PhD
Director of MRI Safety Evaluations and Engineering Simulations
MED Institute
West Lafayette, Indiana, United States- BS
Behzad Sharif, PhD
Associate Professor
Purdue University
Indianapolis, Indiana, United States
Presenting Author(s)
Primary Author(s)
Co-Author(s)
Methods: Based on established work8 on estimating fractional blood volume using T1 maps using intravascular contrast agents, we derived a formula to estimate MBVR. Our method involves a SASHA-like9,10 continuous beat-by-beat T1 mapping during slow ferumoxytol infusion to estimate extravascular T1 (T1ev) at blood-myocardium equilibrium. This value is then used to correct stress/rest FE T1 reactivity measurements, yielding physiologically meaningful MBVR estimates (Fig. 1). Preclinical validation was performed in domestic swine (n=13, weight: 46 ± 5 kg), including both healthy and ischemic models. In a subset (n=8), myocardial ischemia was induced via microsphere embolization under x-ray guidance.7,11 T1 mapping was performed at rest and during adenosine-induced stress. Segment-wise MBVR maps were generated and compared to FE T1 reactivity maps. Diagnostic performance was evaluated using receiver operating characteristic (ROC) analysis on a per-vessel basis.
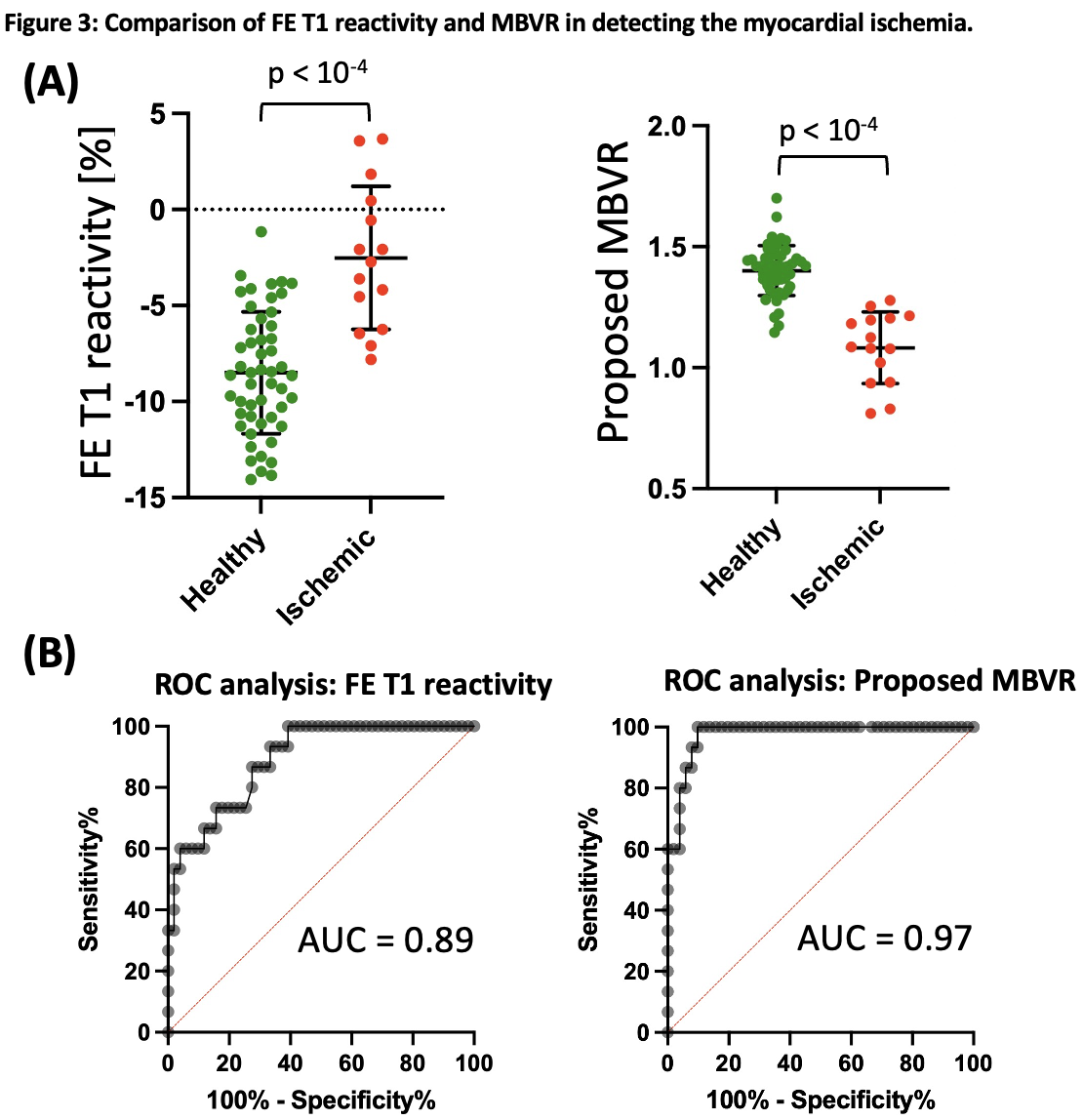
Results: As shown with the representative cases in Fig. 2, FE T1 reactivity and MBVR are uniformly distributed across AHA segments in the healthy case (top row), while in the diseased case (bottom row), both metrics differentiate ischemic severity across vessel territories. Notably, MBVR values in remote territories remained consistent, supporting its dose-independent nature. In healthy vs ischemic regions, mean T1 reactivity was −8.5% ± 3.2% vs −2.5% ± 3.7% (p < 0.01), while MBVR was 1.40 ± 0.10 vs 1.08 ± 0.15 (p < 0.01), as shown in Figure 3a. ROC analysis revealed a significantly higher area under the curve (AUC) for MBVR compared to FE T1 reactivity (0.97 vs 0.89, p < 0.05), indicating improved sensitivity and specificity for ischemia detection (Fig. 3b).
Conclusion: This study introduces a practical, dose-independent method for MBVR quantification using FE-CMR at 0.55T. Our approach enhances the diagnostic utility of FE imaging and enables standardized assessment of coronary microvascular function. The method is compatible with existing protocols and may facilitate broader clinical adoption of MBVR as a reliable biomarker for ischemia.
Figure 1. Overview of the proposed approach for MBV reserve (MBVR) estimation. (A) Ferumoxytol is slowly infused while dynamic T1 mapping—using a pulse sequence available on the scanner (see Methods)—tracks blood and myocardial T1 values on a beat-by-beat basis. Equilibrium T1 is identified when these values align, typically within two minutes of infusion. At this convergence point, the extravascular T1 (T1ev) is determined as the common T1 value shared by blood and myocardium. (B) Following the infusion, T1 maps are obtained both at rest and under pharmacologically induced stress. Instead of assessing the relative T1 change between rest and stress (as done in standard FE T1 reactivity), this method applies the previously derived T1ev to correct the myocardial T1 values at both states. This correction allows for direct MBVR calculation across AHA segments.
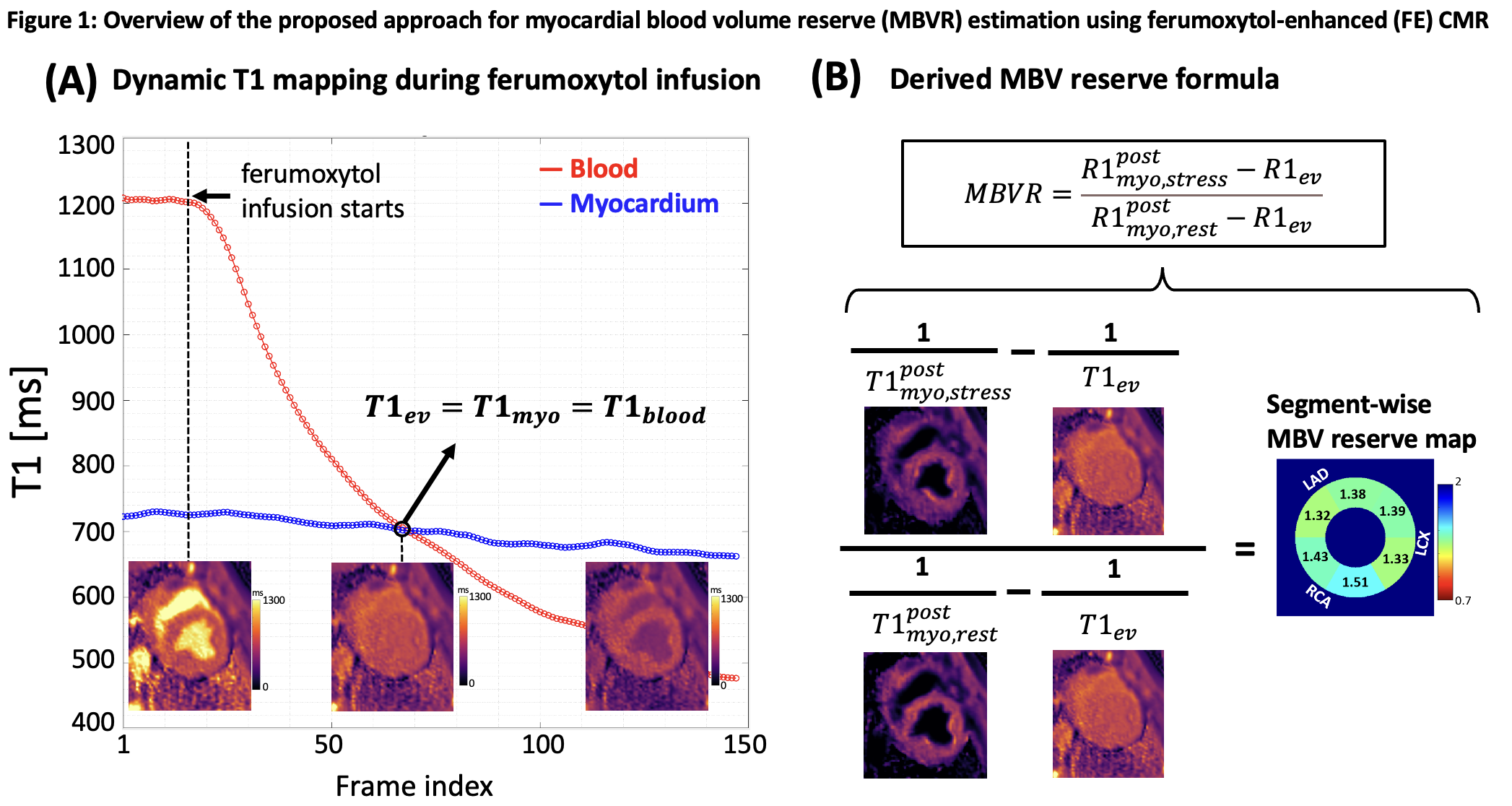 Figure 2. Example in vivo cases showing T1 maps, ferumoxytol-enhanced (FE) T1 reactivity, and MBV reserve (MBVR) in a healthy subject (top row) and one with varying degrees of microvascular disease (bottom row). (A) In the healthy subject, both FE T1 reactivity and MBVR appear relatively consistent throughout the myocardium, with expected physiological variations. (B) In the diseased subject, both metrics clearly distinguish between regions of severe ischemia (LAD), mild ischemia (LCX), and unaffected myocardium (RCA). Importantly, MBVR values in the RCA region remain comparable to those in the healthy case, underscoring its reliability as a physiological biomarker that is independent of dose. In contrast, FE T1 reactivity in the same RCA area shows noticeable differences (nearly −13% vs. −7%), likely reflecting variations in ferumoxytol dosage between the two experiments.
Figure 2. Example in vivo cases showing T1 maps, ferumoxytol-enhanced (FE) T1 reactivity, and MBV reserve (MBVR) in a healthy subject (top row) and one with varying degrees of microvascular disease (bottom row). (A) In the healthy subject, both FE T1 reactivity and MBVR appear relatively consistent throughout the myocardium, with expected physiological variations. (B) In the diseased subject, both metrics clearly distinguish between regions of severe ischemia (LAD), mild ischemia (LCX), and unaffected myocardium (RCA). Importantly, MBVR values in the RCA region remain comparable to those in the healthy case, underscoring its reliability as a physiological biomarker that is independent of dose. In contrast, FE T1 reactivity in the same RCA area shows noticeable differences (nearly −13% vs. −7%), likely reflecting variations in ferumoxytol dosage between the two experiments.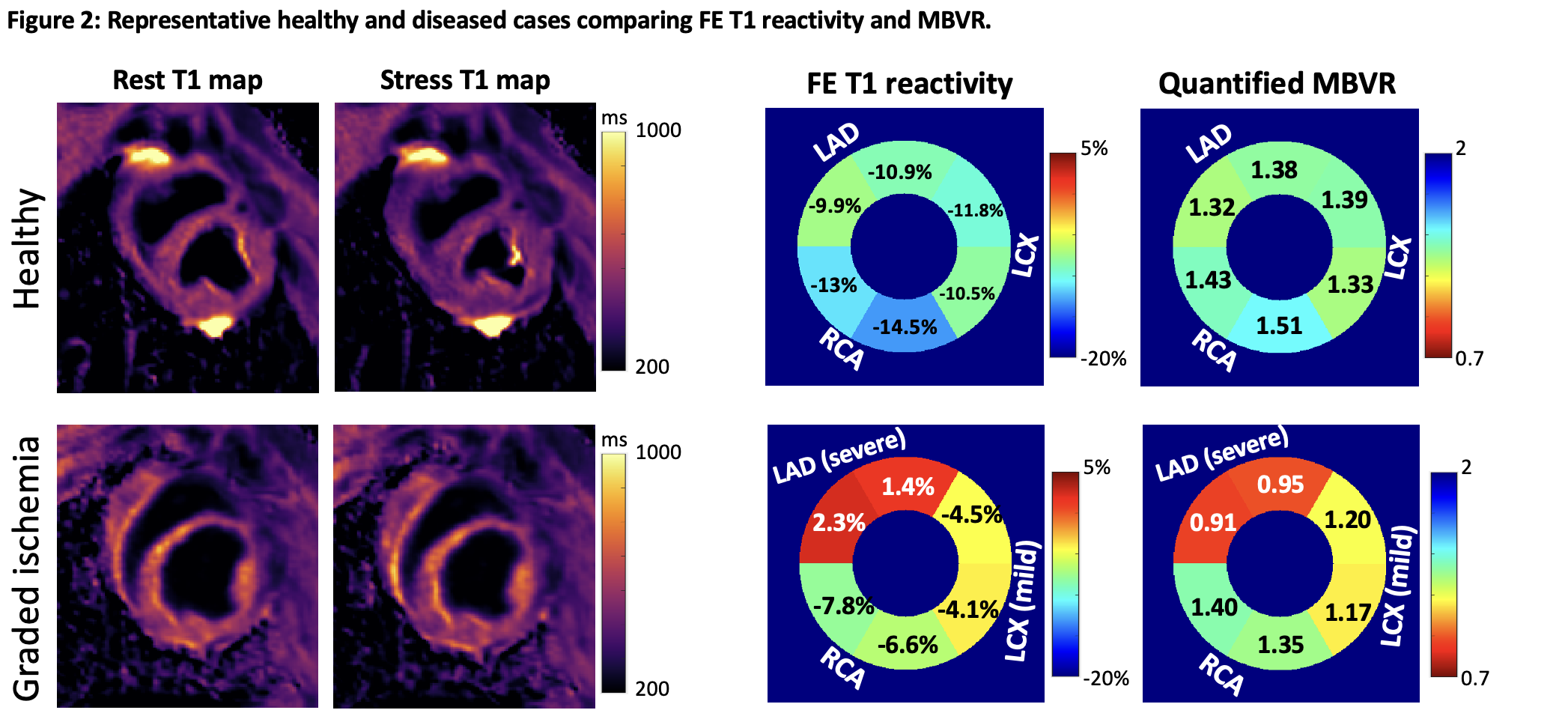 Figure 3. Comparison of in vivo findings highlighting the effectiveness of ferumoxytol-enhanced (FE) T1 reactivity and the proposed MBV reserve (MBVR) in distinguishing between healthy and ischemic myocardial tissue. (A) In regions supplied by healthy coronary arteries (green dots), the average FE T1 reactivity was −8.5% ± 3.2%, whereas ischemic regions (red dots) showed a reduced response of −2.5% ± 3.7%, with a statistically significant difference (p < 10⁻⁴). Likewise, MBVR values were notably higher in healthy areas (1.40 ± 0.10) compared to ischemic ones (1.08 ± 0.15), also with strong statistical significance (p < 10⁻⁴). (B) Receiver operating characteristic (ROC) analysis reveals that MBVR achieves a superior area under the curve (AUC = 0.97) for identifying myocardial ischemia, outperforming FE T1 reactivity (AUC = 0.89), with the difference reaching statistical significance (p < 0.05).
Figure 3. Comparison of in vivo findings highlighting the effectiveness of ferumoxytol-enhanced (FE) T1 reactivity and the proposed MBV reserve (MBVR) in distinguishing between healthy and ischemic myocardial tissue. (A) In regions supplied by healthy coronary arteries (green dots), the average FE T1 reactivity was −8.5% ± 3.2%, whereas ischemic regions (red dots) showed a reduced response of −2.5% ± 3.7%, with a statistically significant difference (p < 10⁻⁴). Likewise, MBVR values were notably higher in healthy areas (1.40 ± 0.10) compared to ischemic ones (1.08 ± 0.15), also with strong statistical significance (p < 10⁻⁴). (B) Receiver operating characteristic (ROC) analysis reveals that MBVR achieves a superior area under the curve (AUC = 0.97) for identifying myocardial ischemia, outperforming FE T1 reactivity (AUC = 0.89), with the difference reaching statistical significance (p < 0.05).