Late Breaking Clinical Trials
Virtual Recording
Ethnic Differences in Cardiac Structure, Function, and Epicardial Fat: Potential Early Life Implications for HFpEF Risk

Suresh Anand Sadananthan, PhD
Research Scientist
A*STAR Institute for Human Development Potential
Singapore, Singapore
Suresh Anand Sadananthan, PhD
Research Scientist
A*STAR Institute for Human Development Potential
Singapore, Singapore- YK
Yeshe Manuel Kway, PhD
Postdoc Research Fellow
University of Oxford, United Kingdom - NM
Navin Michael, PhD
Principal Scientist
A*STAR Institute for Human Development and Potential, Singapore - DO
Delicia Shu Qin Ooi, PhD
Assistant Professor
National University of Singapore, Singapore - FY
Fabian Yap
Professor
KK Women's and Children's Hospital, Singapore - KT
Kok Hian Tan
Professor
KK Women's and Children's Hospital, Singapore - KG
Keith M. Godfrey
Professor
University of Southampton, United Kingdom - YL
Yung Seng Lee
Professor
National University of Singapore, Singapore - PG
Peter D. Gluckman
Professor
A*STAR Institute for Human Development and Potential, Singapore - YC
Yap Seng Chong
Professor
National University of Singapore, Singapore - MF
Marielle Valerie Fortier, MD
Associate Professor
KK Women's and Children's Hospital, Singapore - MD
Mayank Dalakoti
Associate Consultant
National University Heart Centre Singapore, Singapore - SV
S Sendhil Velan
Professor
University of Massachusetts Amherst, United States - JE
Johan Eriksson
Professor
A*STAR Institute for Human Development and Potential, Singapore
Presenting Author(s)
Primary Author(s)
Co-Author(s)
Methods: We analysed cardiac MRI data from 425 children (age 10.5 years; 208 boys, 217 girls; 234 Chinese, 133 Malay, 58 Indian) in the GUSTO study. Left ventricular mass, end-diastolic and end-systolic volume, stroke volume, cardiac output, and ejection fraction (LVMI, EDVI, ESVI, SVI, CI, EF) were quantified using a CINE sequence (TR=39.1 ms, TE=1.37 ms, slice thickness=8 mm) with ECG gating and an 8-second breath-hold on a Siemens Prisma 3T MR scanner. The data were processed using Segment software and indexed to body surface area. EAT was assessed using a T1-weighted dark blood sequence (TR=649 ms, TE=15 ms, slice thickness=7mm, interslice gap=1.05 mm) and quantified through deep learning-based segmentation. The systemic glycosylated inflammatory protein marker GlycA was measured by NMR-based metabolomics. Ethnic differences were examined using ANCOVA adjusted for sex. The association between EAT and GlycA was evaluated using linear regression adjusted for ethnicity, sex, BMI, and maternal education.
Results:
Indian children exhibited smaller LV mass and ventricular volumes (EDVI, ESVI, SVI) compared to Chinese and Malay children (Fig. 1), suggesting a slower cardiac growth trajectory or adaptive mechanisms that preserve EF despite reduced chamber size. Chinese and Malay children exhibited larger hearts and higher LV volumes, possibly reflecting more robust growth or early adaptation to greater metabolic demands. EF was preserved across all ethnicities, indicating maintained systolic function despite structural differences.
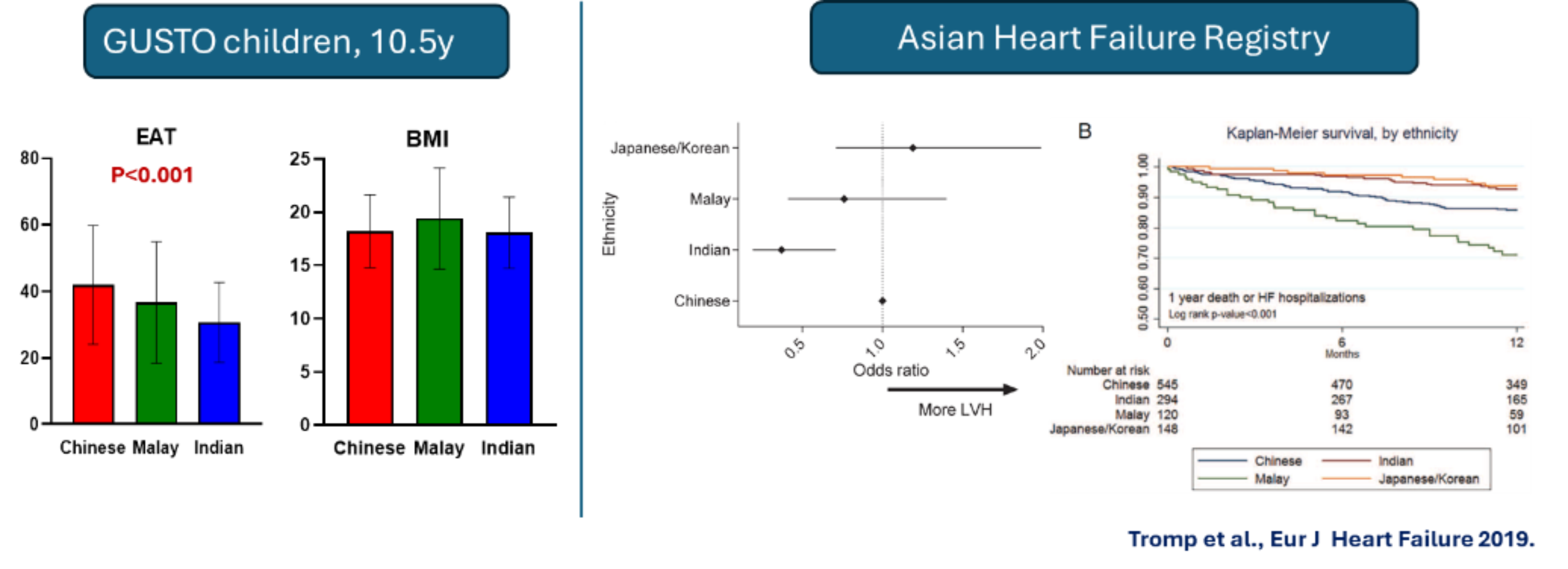
Despite similar BMI, Chinese children had higher EAT (41.9±17.8 cc) than Malay (36.6±18.3 cc) and Indian (30.7±12.0 cc) children (Fig. 2). The higher EAT in Chinese children was consistent with adult data from the Asian Heart Failure Registry showing greater prevalence of heart failure with preserved ejection fraction (HFpEF) in Chinese adults compared to Malays and Indians. EAT was positively associated with GlycA (β=0.001 mmol/L; CI=0.0004, 0.002; p=0.002) independent of BMI.
Conclusion:
The positive BMI-independent association of EAT with GlycA highlights its potential inflammatory role in the pathogenesis of cardiometabolic disease. These early observations of higher EAT and cardiac size in Chinese children may serve as subclinical markers of future cardiovascular risk, especially if obesity or metabolic syndrome develops in adulthood.
Figure 1. Ethnic differences in cardiac structure and function in GUSTO children at age 10.5 years 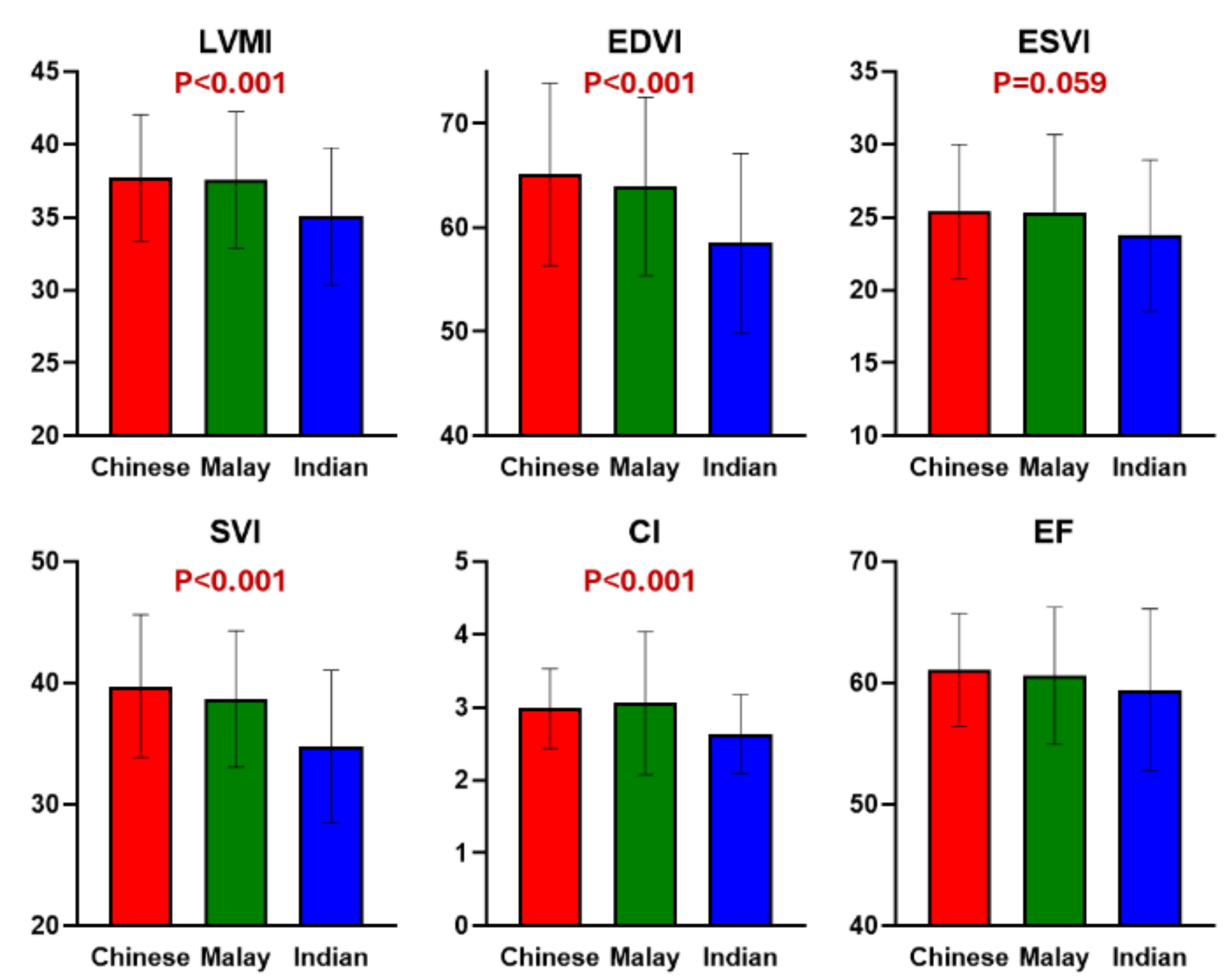 Figure 2. Ethnic differences in epicardial fat (GUSTO children) and HFpEF prevalence (Asian Heart Failure Registry)
Figure 2. Ethnic differences in epicardial fat (GUSTO children) and HFpEF prevalence (Asian Heart Failure Registry)